The United States is the only industrialized nation without universal health insurance coverage, and reducing the proportion of uninsured Americans in the absence of national health insurance has proven to be an elusive goal. In 2000, at the very height of the economic boom, 39 million Americans (14% of the population) lacked coverage. Women of reproductive age bear a disproportionately large share of the burden: Nearly one in five have neither private insurance nor Medicaid coverage, and the proportion of reproductive-age women covered by Medicaid has been dwindling for several years (see chart below).
| Coverage Trends |
| Nearly one in five women of reproductive age are uninsured, while the proportion covered by Medicaid has fallen in recent years. |
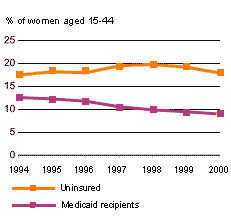 |
|
Source: The Alan Guttmacher Institute, tabluations of data from U.S. Census Bureau Current Population Surveys, 1995-2001. |
Enter HIFA
Following the demise of the Clinton administration's ill-fated push for large-scale health care reform in the early 1990s, federal policy initiatives have been modest and targeted. The Health Insurance Portability and Accountability Act of 1996 sought to prevent people from losing coverage when they change jobs, while the 1997 State Children's Health Insurance Program (SCHIP) focused on expanding coverage for children in families with incomes up to 200% of poverty ("The New Children's Health Insurance Program," TGR, April 1998 ).
In August 2001, the Bush administration unveiled its Health Insurance Flexibility and Accountability (HIFA) demonstration initiative, designed to encourage "new comprehensive state approaches" to reducing the number of uninsured Americans, largely through Medicaid. Under HIFA, states could seek waivers from the Centers for Medicare and Medicaid Services (CMS), the federal agency that administers Medicaid, to extend a limited package of benefits to people who would not otherwise be eligible. States could cover these enrollees only for basic primary care.
From the very beginning, the new initiative raised concerns from a wide-ranging coalition of advocates working to ensure access to services under Medicaid for low-income children, families and disabled Americans. Covering new populations, even for a modest set of services, inevitably would cost money, and Medicaid waivers, including those under HIFA, must be budget-neutral to the federal government (that is, federal spending under a waiver cannot exceed what federal spending would have been without a waivers). Therefore, advocates feared that expansions could lead to cuts in services or increases in cost-sharing for current Medicaid recipients. Reproductive health advocates were concerned from the outset, since 9% of all U.S. women of reproductive age rely on Medicaid for their care and family planning is among the handful of services to which all Medicaid recipients are entitled under federal law (see box, below).
HIFA spells out three possible ways for states to finance expansions. First, states could divert unspent funds remaining from their allotments under SCHIP. Second, they could redirect funds earmarked for so-called disproportionate share hospitals—facilities that receive supplemental Medicaid payments in return for serving a high proportion of high-cost, low-income patients. Third, states could reduce benefits and/or increase cost-sharing to some current Medicaid enrollees.
Under HIFA, states would not be able to cut the core package of benefits that are federally mandated for specific "mandatory" groups of people enrolled as a result of a direct requirement in federal law. (These populations include pregnant women and children in families with incomes up to limits set in federal law and parents of enrolled children with incomes up to state-set income limits.) HIFA, however, would permit states to cut the benefits (even from the core package) or increase the cost-sharing of people enrolled at a state's option. These "optional" enrollees include the same groups of people, but with incomes too high for them to qualify for mandatory coverage, such as pregnant women and young children in families with incomes above 133% of the federal poverty line ($15,020 for a family of three), older children of families with incomes over 100% of poverty and children covered under SCHIP.
State Demonstration Plans
In the year since HIFA was unveiled, 11 states have submitted proposals (see table); six plans—from Arizona, California, Illinois, Maine, New Mexico and Utah—have been approved. (The proposal from Utah technically was not submitted under the HIFA initiative, but it is consistent with HIFA's goals and structure and is considered part of the effort for purposes of this analysis.)
| PENDING AND APPROVED HIFA WAIVERS | |||||||||
| State | Major Expansion Populations | Funding Sources for Expansion | |||||||
| Parents | Child-less Adults | Other | SCHIP | DSH* | Benefit Cuts | Cost-Sharing | Enrollment Fee | Enrollment Cap | |
| APPROVED | |||||||||
| Arizona | X | X | X | ||||||
| California | X | X | |||||||
| Illinois | X | X | |||||||
| Maine | X | X | |||||||
| New Mexico | X | X | X | ||||||
| Utah | X | X | X | X | X | ||||
| PENDING | |||||||||
| Colorado | Pregnant Women | X | |||||||
| Delaware | Transitional Medicaid | X | X | X | |||||
| Michigan | X | X | Pregnant Women | X | X | X | X | ||
| Oregon | X | X | Children | X | X | X | X | ||
| Washington | X | X | X | X | X | X | X | ||
| *Disproportionate Share Hospital payments. Not technically part of HIFA program. | |||||||||
The plans' goals are laudable: Eight, including five of the six that have been approved, seek to cover parents of enrolled children, while seven would bring childless adults into Medicaid. Some states are looking to enroll other populations, such as pregnant women and children in families with higher incomes, or families whose temporary Medicaid coverage is running out. Still, the experience with HIFA has not only borne out advocates' fears of cuts but also raised the profile of concerns about diverting money allocated to cover children under SCHIP.
To cover the costs of these expansions, states are seeking to utilize the full array of options given to them under HIFA, and then some. Five states would include benefit cuts to existing enrollees, most often to pharmacy, home health, dental care and mental health services; four of the five states would also charge enrollment fees or impose additional cost-sharing for beneficiaries. Two states are seeking to use funds earmarked for disproportionate share hospitals to pay for their efforts.
But by far, the most common source of funds designated by states is SCHIP. Because the program is relatively new and has gotten off to a slow start, many states have not spent the entire amount of federal SCHIP funds allocated. Four of the six states with approved waivers and all five states with pending proposals would rely on unspent SCHIP funds to pay for their expansions; in five states, including four with approved waivers, SCHIP is the only funding source contemplated by the state.
Diverting SCHIP Funds
As would be expected, the reliance on SCHIP to fund HIFA waiver programs is controversial. Advocates and policymakers of both parties have expressed dismay at the extent to which SCHIP funds are being relied upon and the purposes for which they are being used. These questions are outlined in detail in a recent report from the General Accounting Office (GAO), the nonpartisan investigative arm of Congress. Indeed, the report, which was prepared at the request of Sen. Max Baucus (D-MT), chairman of the powerful Senate Finance Committee that has jurisdiction over both Medicaid and SCHIP, found HIFA lacking from several perspectives.
The GAO report charged that CMS has failed to provide adequate opportunity for public participation in the decision making process, even though there is a clear Department of Health and Human Services (DHHS) policy dating from the mid-1990s that outlines a process for public involvement. The report also included specific suggestions for legislation to remedy the problem.
The GAO explicitly criticized HIFA's use of SCHIP monies to fund coverage expansions for adults despite what the GAO said was Congress's clear intention that program funds should, in most cases, be used to cover children. In the event that a state does not use its entire SCHIP allotment, Congress specified that most of the unused monies be redistributed to states that have used up their allocations (in April, CMS reallocated $1.6 billion to 18 states and territories). According to the GAO, giving states wide latitude to use unspent SCHIP funds for adults could pit adults against children—something Congress never intended.
The GAO pointed out that under the SCHIP statute, a state may obtain federal permission to cover parents only if it can demonstrate that the cost of covering both children and parents would be less than the cost of covering just children—a hurdle not cleared by the states in the HIFA process, according to the report. The GAO therefore called on Congress to clarify whether the cost-effectiveness standard could be waived in this situation. Furthermore, the statute makes no provision whatsoever for the coverage of childless adults. In that light, the GAO report calls on Congress to amend SCHIP to explicitly prohibit using program funds to cover adults without children and on CMS to amend current and pending waivers to block using SCHIP monies for this purpose.
Almost immediately after receiving the report, Baucus, along with Sen. Chuck Grassley (R-IA), the Finance Committee's ranking Republican, wrote DHHS Secretary Tommy G. Thompson, saying that the nation's five million uninsured children "should never have to compete with childless adults for the use of remaining SCHIP funds." They called on Thompson to discontinue the practice, and warned of "legislative action to end this violation of Congressional intent," if it did not happen expeditiously. In a letter responding to the GAO report published in USA Today, Thompson voiced his continued support for the effort saying that "children remain the first priority for the SCHIP program, and no child will go without coverage because funds went to an adult. But we can also use these funds in innovative ways to expand access for adults. That's what many states want to do, and we support them."
Outlook Bleak for States
At the same time the GAO is challenging what has come to be HIFA's major funding source, states are facing bleak economic times; Medicaid, which currently accounts for about one-fifth of all state spending, is a major component of the problem. Operated and funded jointly by the federal government and the states, Medicaid currently subsidizes the health care of 10% of all Americans. The program is specifically designed to grow during lean economic times—as welfare rolls grow, so do the number of people eligible for Medicaid.
According to the National Conference of State Legislatures, 29 states have seen welfare caseload increases of more than 6% over just the last two years. The resulting increases in Medicaid spending have serious economic implications for the state budgets: According to the National Association of State Budget Officers, 39 states had shortfalls in their Medicaid budgets last year and 28 expect to find themselves in a similar position this year. "As it stands," commented Idaho Gov. Dirk Kempthorne (R), vice chairman of the National Governors Association, "states can no longer afford Medicaid."
With states generally required to have balanced budgets, they have been searching for a way out ("Post-Attack Economic Woes Create Challenges for Family Planning Advocates," TGR, December 2001, page 8). In July, the Senate passed a measure to temporarily increase the share of Medicaid costs paid by the federal government, a move that would considerably reduce the burden borne by the states. While the measure may yet see further action in Congress this year, some states have already moved to cut Medicaid expenditures, and more plan to do so. In June, Health Management Associates found that 41 states reported plans to cut Medicaid, including putting controls on pharmacy costs, increasing cost-sharing, eliminating optional benefits and reducing eligibility; 17 states reported plans to submit waivers under HIFA to allow structural changes to their programs.
It is little wonder that advocates continue to monitor the HIFA process closely and with some skepticism. Indeed, ever since the administration initially announced HIFA last year, advocates have been expressing concerns that the requirement for budget neutrality could lead to benefit cuts for current enrollees. According to the Urban Institute, the group affected by such cuts would be sizable, encompassing close to 30% of all Medicaid recipients and including four in 10 enrolled parents. For them, charges Mara Youdelman of the National Health Law Program, "HIFA waivers are nothing more than a benefit cut in disguise."
Also from HIFA's unveiling, advocates had noted with alarm that although CMS officials had stated publicly that any cuts to state Medicaid programs would be used to provide at least some coverage to individuals in the state who lacked any insurance at all, the official guidance released by the agency did not make this an explicit requirement. They reasoned that the economic boom of the 1990s could not continue indefinitely and that states soon would begin to feel the squeeze in their Medicaid programs. With states facing a bleaker economic situation now than even little more than a year ago, a draft letter to Secretary Thompson from Montana Gov. Judy Martz (R) put advocates' fears squarely on the table. The draft, posted on the National Health Law Program's Web site, indicates the governor's intention to submit an application for a HIFA waiver that would make cuts to the state's Medicaid program without any concomitant coverage expansion whatsoever.
HIFA's Implications for Family Planning
Family planning has long had a special status in the Medicaid program. In 1972, Congress expanded the small package of benefits for which Medicaid recipients in all states are covered to include "family planning services and supplies furnished (directly or under arrangements with others) to individuals of childbearing age (including minors who can be considered to be sexually active) who are eligible under the state [Medicaid] plan and who desire such services and supplies." This move established a legal entitlement to family planning for Medicaid recipients nationwide. Federal law also prohibits states from charging fees to enrollees seeking family planning care.
Although these two mandates remain in effect, reproductive health advocates are concerned that states, under HIFA, could limit these guarantees to only the so-called mandatory populations and exclude family planning coverage for optional populations. Alternatively, states could continue coverage for family planning but impose fees for optional enrollees obtaining the services. So far, none of the HIFA plans seem to either exclude family planning or assess fees. However, in an ominous move, Utah's plan does require cost-sharing for emergency services, which, like family planning, historically had been exempt from fees.
When it comes to the expansion populations being covered under state HIFA plans, advocates are worried that the discretion given states to limit coverage to only basic primary care might result in the exclusion of family planning. So far, at least, none of the state plans appear to do so, although Utah's plan explicitly says that while family planning in general is covered, Norplant (which is no longer being marketed in the United States) and infertility treatment are excluded. While reassured by the current plans' seeming inclusion of family planning for optional and expansion groups, advocates remain mindful that the proposals submitted to—and, in some cases, approved by—CMS are just the initial blueprints for the state efforts. They also are aware that it is critically important to track these efforts at every step of the implementation process to ensure that the long-standing entitlement to family planning services for Medicaid enrollees is not diminished through the HIFA initiative.

